Many people are still familiar with the concept of the traditional family doctor. For a long time, GPs in Switzerland were as much a part of the fabric of local life as members of the clergy. They were more commonly male than female, and their practices were almost always open. You could contact them at night, at weekends and at Christmas. They would visit you at home and care for your entire family, young and old. Their wives would hold the fort for them, managing the children and the household. Later one of their sons would inherit the practice, where possible. Yet this is increasingly becoming a thing of the past.
Family doctors who wish to retire due to age now have a hard time finding someone to take over their practice – particularly in rural areas or peripheral regions. Many of them delay their retirement and carry on until they are 70. This situation may get even worse. Some 19,000 doctors work in the outpatient sector, 40 per cent of whom are general practitioners. The average age of GPs in Switzerland is 55. Many are about to retire. Meanwhile, demand for medical care is likely to increase amid an ageing population and a rise in chronic illnesses (see additional text). A study by the University of Basel warns that Switzerland already has a shortfall of 2,000 GPs. This figure could double in the future.
The backbone of primary care
Family doctors in Switzerland are important because, as general practitioners, they form the backbone of primary care. At 4.3 per thousand inhabitants, Switzerland actually has a high density of doctors compared to other countries (hospital physicians included). However, the spread of doctors around the country is uneven. The urban canton of Basel-Stadt has 10.1 doctors per thousand inhabitants, while the mountainous canton of Uri only has 1.8. Divergent trends also come into the equation. On the one hand, there is a shortage of GPs. On the other hand, entry restrictions are designed to prevent too many independent doctors from practising. This particularly applies to the more expensive specialists who work in urban areas. Thus, there is a danger of having at the same time a lack of doctors and a surplus of doctors.
One thing that is clear, however, is that healthcare costs in Switzerland are increasing year by year. Switzerland’s mandatory health insurance premiums reflect this. Policymakers have difficulty curbing the rise in costs. This is due, not least, to the complicated Swiss healthcare system that involves both state intervention and the free market, and features numerous stakeholders and varied interests – from the federal government, the cantons and municipalities, to doctors, hospitals, health insurers and patients.
Protest outside parliament
Switzerland’s GPs lost patience in 2006. When the then health minister Pascal Couchepin (FDP) introduced a plan to reduce laboratory tariffs, it led to unusual scenes in Berne. Thousands of doctors took to the streets for the sake of their profession, demonstrating in front of the Federal Palace. The “Yes to family medicine” popular initiative also helped to exert pressure. In 2014, the electorate voted very clearly in favour of a counter-proposal to this initiative. This granted constitutional status to general practice medicine, meaning that the federal government and the cantons must now ensure adequate provision of high-quality primary healthcare and promote the GP profession as a key component in this regard. A master plan initiated by Couchepin’s successor Alain Berset (SP) gave GPs a better deal on tariff issues, while education and further training were also improved.
Has this been the right medicine? And why were ever fewer young doctors deciding to become GPs in the first place? We went to Berne’s university quarter to find out. Professor Sven Streit works at the university’s Institute of Primary Health Care (BIHAM), which was founded in 2009. The fact that primary care is now treated as an academic discipline is part of the solution, he believes. “GPs had an image problem within the medical profession.” They were regarded as practitioners who were far removed from the research environment.
Training the GPs of tomorrow
“This was completely unjustified,” he adds, pointing out that GPs have a broad range of knowledge and rely on research findings just as much as specialists who work at central hospitals. Four professors now teach and carry out research at BIHAM on issues such as high blood pressure or the provision of care to elderly people with multiple illnesses. BIHAM also focuses on training the GPs of tomorrow – and its efforts are beginning to pay off. “Some 20 per cent of medical students say that they want to become GPs – twice as many as ten years ago,” says Streit.
This is probably because prospective doctors are now sent out during their studies to do work experience at a general practice. As part of their specialist training after graduation, they also have the chance to do an assistantship at a GP surgery, with the cantons subsidising a portion of their salaries. For example, the canton of Berne pays 1.5 million Swiss francs to 35 GP trainees each year. Streit says that 80 per cent of those who do an assistantship go on to become GPs. “These practical insights are important.” They lend a fresh image to the profession.
No more going it alone
For Streit, the attraction of working as a GP is the human side of being close to your patients and focusing holistically on their needs. Not only that, but GPs also have different working conditions nowadays. Younger doctors no longer want to be on call seven days a week as their predecessors were, he explains. They prefer more structured working hours. Many like working part-time for a better work-life balance. The proportion of female doctors is increasing, with more women than men now studying medicine. This is probably one of the reasons why group practices are becoming more popular. Such set-ups allow doctors to share the workload including emergency on-call commitments, as well as infrastructure and administrative tasks. Over half of GP practices in Switzerland are still individual practices, but the number of group practices has tripled in recent years. Streit is unequivocal: “The structural shift will continue.”
Older doctors are also discovering the benefits of being part of a group practice. One them is Philippe Luchsinger, Chairman of the Association of Swiss General Practitioners and Paediatricians (MFE). The GP practice that Luchsinger took over in Affoltern am Albis (canton of Zurich) more than 30 years ago is now a group practice. “We need to get away from the image of a GP as someone who goes it alone,” he says, adding that the GPs of tomorrow are team players who are also seeking to collaborate with paramedical professionals such as nurses, physiotherapists and pharmacists. Although voters decisively rejected a proposal in favour of “managed care” systems in 2012, experts believe that the future lies in coordinated care.
Advanced practice nurse relieves workload
What does coordinated care look like in practice? One example is the Medizentrum group practice in the rural municipality of Schüpfen (canton of Berne), where Christine Wyss works as an advanced practice nurse (APN) together with a team of GPs. Wyss, who graduated with a master’s degree, has an extended range of responsibilities. “My main focus is on older, chronically ill patients who need long-term care,” she says. Wyss makes herself available for consultations. She also administers infusions to patients, takes their pulse and blood pressure, discusses laboratory results with them, and gives them advice. In addition she visits elderly patients who are no longer as mobile as they used to be. Her duties include tasks traditionally carried out by doctors, but the scope of her activity is defined by the GP.
“She is much more qualified than me in other areas,” says Hansulrich Blunier, a GP colleague at the Schüpfen practice with many years’ experience. For example, Wyss is able to teach patients how to cope with their illnesses on a day-to-day basis. This frees Blunier up to deal with more complex cases. Medizentrum offers procedures such as gastrointestinal endoscopies as well as chemotherapy. Blunier thinks that this arrangement enhances his profession. This work is pioneering because APNs in Switzerland still do not have an official job description. There is no official billing tariff either. Uri – a canton with numerous valley communities that have been hit particularly hard by the shortage of GPs – has now launched a three-year APN pilot project.
Virtual GPs?
Or is the future of GP practices online? Yes, says specialist physician Andrea Vincenzo Braga during a Skype call. Braga is Chief Medical Officer at eedoctors, a Berne start-up that was established in 2017. “Digital platforms can play a part in outpatient primary care,” he says. Patients can access eedoctors via a smartphone app and get medical advice through a video link. Prescriptions are sent directly to their smartphones. “We fill a gap in the market whenever GPs aren’t available,” says Braga. This can be when they are on holiday, or in areas of the country where relatively few GPs operate. Braga says that his service is also a handy option for professionals with limited time, particularly as people commonly work and live in different places nowadays. More than 20 doctors work for eedoctors – from home. Braga believes that primary care must move with the times because many GP consultations do not even require doctor and patient to be in the same room.
According to Professor of Primary Care Sven Streit, Switzerland probably needs a variety of solutions (e.g. new communication channels, new practice models) to reflect its regional diversity. “No two regions are the same,” Streit says. He thinks that the tide has turned in addressing the shortage of GPs. Philippe Luchsinger is also delighted about increased levels of interest among young people. “Primary care is sexy again,” he says. However, he warns that Switzerland cannot afford to rest on its laurels. It will still take years before the medical students who are interested in primary care actually become GPs. Until then, Switzerland will continue to be short of family doctors.
An ageing population, more chronic illnesses
Switzerland’s population is getting older. According to the Federal Statistical Office, the number of inhabitants over 65 is likely to rise from 1.5 million to 2.7 million by 2045. The growing proportion of elderly people, not to mention the modern lifestyle characterised by smoking, an unhealthy diet and too little exercise are leading to an increase in chronic illnesses such as cancer, diabetes, cardiovascular disease and dementia. Many older people suffer from several illnesses at the same time. Chronic illnesses now account for the biggest share of Switzerland’s 80-billion-franc annual healthcare bill.
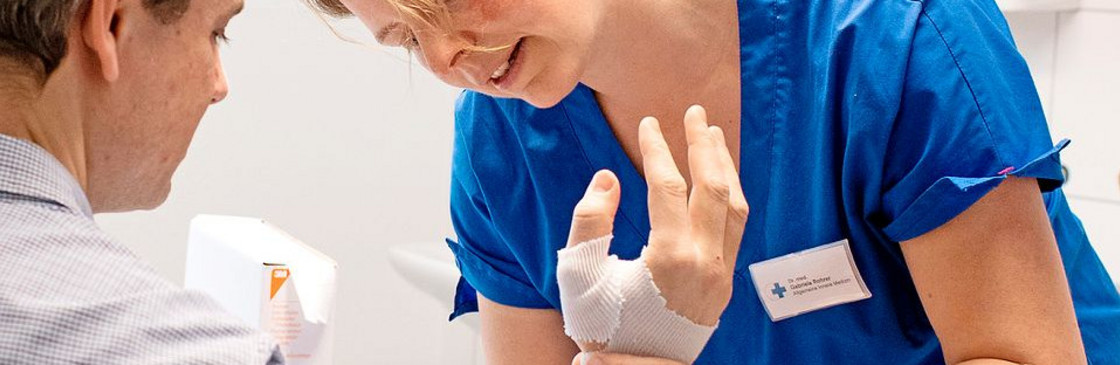
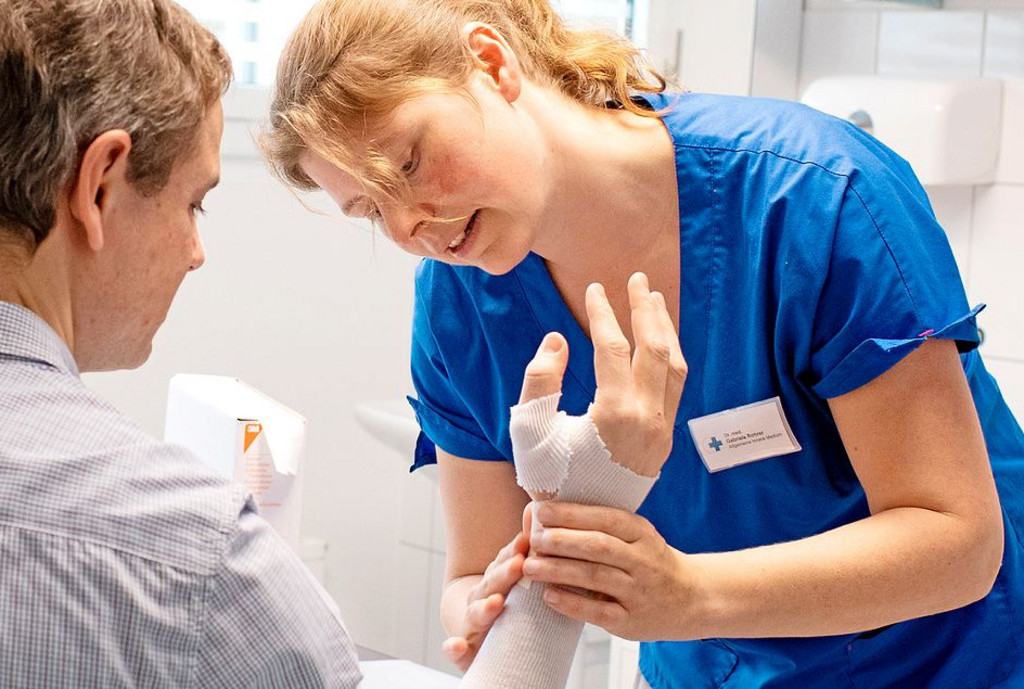
Interview on this topic: “A wonderful job”












Comments
Comments :
Ich würde sofort freiwillig und kostenlos ein kleines Dorf in Uri auf den Weg der Gesundheit bringen, wenn man mir dies erlauben würde. Ich bin kein Doktor, aber bein Vater war einer und ich habe von ihm, wie auch vom ehemaligen Dr. med. Ernst Bauer in Arosa das Heilen gelernt. Mein Vater praktizierte nie Medizin, er sagt es sei der grösste Betrug des Jahrhunderts, er könne da nicht mitmachen. Dafür baute er Spitäler. Diese wird man vermehrt brauchen sagte er, wenn die Medizin so weiter macht. Nebenbei: Krankheiten haben nichts mit dem Alter zu tun!!!
Seit 20 Jahren lebe ich mit meiner Familie in Costa Rica
Thank you for a wonderful article.
A General Practitioner is encountered at the first stage, and one who is trained in Functional Medicine will be one of the most important people in the route to resolving health issues. In the UK, we have a great example in Dr Rangan Chatterjee, who has appeared on BBC TV in two series called "Doctor in the House" where he used Functional Medicine techniques to successfully deal with chronic illnesses and conditions that most doctors consider to be irreversible and/or only 'manageable' with drugs.
I think younger people are more interested in that kind of medical training which involves detailed nutritional expertise and prescribing lifestyle changes to their patients to help them back to health.